Hysterectomy: Purpose, Procedure, Benefits, Risks and Recovery
What is a Hysterectomy ?
Hysterectomy is a surgical procedure that involves the removal of the uterus, and often, the cervix as well. Depending on the medical indication, this surgery may also involve the removal of adjacent organs and tissues, such as the fallopian tubes and ovaries. After a hysterectomy, a woman cannot become pregnant, and she will no longer experience menstrual periods. This procedure is commonly performed to address various conditions affecting a woman’s reproductive system.
In the United States, approximately half a million hysterectomies are conducted annually, making it the second most frequent surgical procedure for women, following cesarean section. Most hysterectomies are performed in individuals aged between 40 and 50.
Indications for Hysterectomy

Hysterectomies are performed by healthcare providers to address various conditions, including:-
- Abnormal or excessive vaginal bleeding that has not responded to other treatment methods.
- Severe menstrual pain that has not been relieved by alternative treatments.
- Leiomyomas or uterine fibroids (benign tumors).
- Persistent pelvic pain related to the uterus that has not improved with other therapies.
- Uterine prolapse, where the uterus descends into the vaginal canal or outside the vagina due to weakened support muscles, resulting in urinary incontinence or bowel movement difficulties.
- Cervical or uterine cancer or precancerous abnormalities for cancer prevention.
- Conditions affecting the uterine lining, such as hyperplasia, recurrent uterine polyps, or adenomyosis.
- Gender affirmation surgery for transgender males.
Different Types of Hysterectomy
The type of hysterectomy required depends on the specific medical condition. The various types of hysterectomy include:
- Total Hysterectomy Removal of the uterus and cervix, while the ovaries are preserved.
- Supracervical Hysterectomy Removal of only the upper part of the uterus, leaving the cervix intact.
- Total Hysterectomy with Bilateral Salpingo-Oophorectomy Removal of the uterus, cervix, fallopian tubes (salpingectomy), and ovaries (oophorectomy). If menopause has not yet occurred, removal of the ovaries may induce menopausal symptoms.
- Radical Hysterectomy with Bilateral Salpingo-Oophorectomy A more extensive procedure involving the removal of the uterus, cervix, fallopian tubes, ovaries, the upper part of the vagina, as well as adjacent tissues and lymph nodes. This type of hysterectomy is typically performed when cancer is present.
Surgical Approaches for Hysterectomy
Hysterectomy, the removal of the uterus, can be performed using different surgical approaches. The two primary methods are traditional open surgery and minimally invasive procedures (MIP).
Open Surgery Hysterectomy
An abdominal hysterectomy is an example of open surgery, representing approximately 54% of hysterectomies for non-cancerous (benign) conditions. In this procedure, a surgeon makes a 5- to 7-inch incision, either vertically or horizontally, across the abdomen to access and remove the uterus. Afterward, patients typically spend 2-3 days in the hospital, with a visible scar as a result of the incision.
Minimally Invasive Procedure (MIP) Hysterectomy
Minimally invasive procedures offer several approaches:
- Vaginal hysterectomy The surgeon makes an incision in the vagina to remove the uterus, leaving no visible scar. Dissolvable stitches are used inside the vagina. This approach is commonly employed for uterine prolapse and nonmalignant conditions, offering the fewest complications and a quicker recovery, usually up to four weeks.
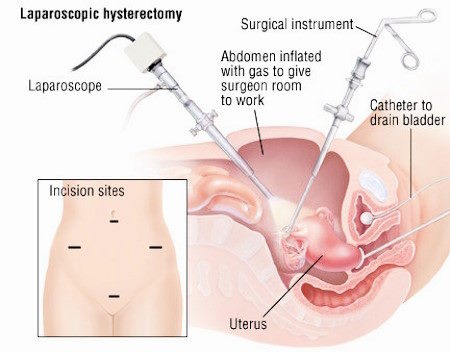
- Laparoscopic hysterectomy This method employs a laparoscope, a tube with a camera and surgical tools, inserted through small abdominal incisions. The surgeon performs the procedure while viewing it on a video screen, and the uterus can be removed in pieces through the incisions. Some patients can go home the same day or after one night in the hospital, and recovery is typically shorter and less painful than with an abdominal hysterectomy.
- Laparoscopic-assisted vaginal hysterectomy Laparoscopic tools in the abdomen are used to assist in removing the uterus through a vaginal incision.
- Robot-assisted laparoscopic hysterectomy Similar to laparoscopic hysterectomy, this approach involves a surgeon controlling a robotic system of surgical tools. Advanced technology allows for natural wrist movements and a 3-dimensional view. Robotic arms and instruments are manipulated by the surgeon using advanced technology that allows for natural wrist movements and a 3-dimensional view.
Opting for minimally invasive approaches for uterus removal offers several advantages over traditional open surgery. Generally, Minimally Invasive Procedure (MIP) result in a faster recovery, shorter hospital stays, reduced pain and scarring, and a lower risk of infection.
Pros and Cons of Hysterectomy
- Hysterectomy can significantly improve a person’s quality of life, especially for those experiencing chronic pelvic pain or severe, irregular bleeding. For individuals at higher risk of uterine cancer, a hysterectomy can reduce this risk and potentially be life-saving.
- Hysterectomy is a major surgical procedure with an extended recovery period. It carries risks, side effects, and is irreversible. Depending on the surgery type, it may induce menopause or menopausal symptoms, and pregnancy becomes impossible after the procedure.
Hysterectomy Procedure and Recovery Details
Preparing for a hysterectomy involves a detailed explanation of the procedure, including potential complications and side effects, by your healthcare provider. Feel free to discuss any concerns you may have, and you may be required to provide blood and urine samples. During the surgery, your healthcare provider will select the most appropriate type of hysterectomy and surgical technique for your specific situation. You will change into a hospital gown and be connected to monitors to track your heart rate. An intravenous (IV) line will be placed in your arm to administer medications and fluids. An anesthesiologist will administer either general anesthesia, during which you will be unconscious throughout the procedure, or regional anesthesia (epidural or spinal anesthesia), where medications are injected near the lower back nerves to block pain while you remain awake.
Procedure Duration
A hysterectomy typically lasts one to three hours, although the duration may vary depending on factors such as the uterus’s size, the need to address scarring from previous surgeries, and the removal of additional tissue or organs (e.g., fallopian tubes or ovaries).
Side Effects/complications
Common side effects of a hysterectomy include vaginal drainage (which may occur for up to six weeks post-surgery) and irritation at the incision sites. If ovaries were removed, menopausal symptoms like hot flushes, vaginal dryness, decreased libido, and insomnia may occur. Infections ,bleeding, injury to bladder and bowel, blood clots and anesthesia related complications are less common but serious risks. Your doctor can discuss treatment options for managing these symptoms.
Post-Hysterectomy Hospital Stay
Hospital stay duration varies depending on the type of surgery. Abdominal hysterectomies may require a few days in the hospital, while vaginal and laparoscopic procedures are less invasive and often do not necessitate an overnight stay. After surgery, walking is encouraged to prevent blood clots in the legs. Recovery instructions, including activity restrictions, will be provided by your healthcare provider.
Recovery Time After a Hysterectomy
The recovery period following a hysterectomy typically ranges from four to six weeks. The duration of recovery depends on the type of hysterectomy performed. Vaginal and laparoscopic hysterectomies generally require less time for recuperation compared to abdominal hysterectomies.
Home Recovery Considerations
The timeline for recovery varies: vaginal and laparoscopic procedures typically necessitate two to four weeks, whereas abdominal hysterectomies may require up to six weeks. Before leaving the hospital, consult with your healthcare provider for personalized instructions on self-care.
Common Post-Hysterectomy Instructions
- Vaginal Bleeding Light vaginal bleeding can persist for one to six weeks. Employ only a light panty liner or sanitary pad to manage the discharge.
- Heavy Lifting Avoid lifting heavy objects (over 10 pounds) for at least four to six weeks.
- Vaginal Rest Abstain from inserting anything into your vagina for four to six weeks, unless otherwise directed by your healthcare provider.
- Sexual Activity Refrain from sexual activity for six weeks post-surgery.
- Hygiene You may shower, and you can cleanse the incision with soap and water. Stitches will dissolve within about six weeks. Bandages over the incision are unnecessary; surgical strips, if used, typically fall off within a week. Staple removal, if applicable, will be done by your healthcare provider.
- Driving You can resume driving about two weeks after abdominal surgery or once you’re no longer taking pain-relieving medications. For vaginal or laparoscopic hysterectomy, driving may be possible within a few days.
- Exercise Gradually reintroduce your exercise routine over four to six weeks, depending on your comfort level.
- Return to Work Depending on your job’s demands, you can typically return to work within three to six weeks.
When to Seek Medical Attention
If you have had a hysterectomy, promptly contact your healthcare provider if you experience:
- Bright red vaginal bleeding.
- A fever exceeding 100 degrees Fahrenheit (37.77 degrees Celsius).
- Severe nausea, vomiting, or difficulty urinating.
- Burning sensation, frequent urination, or difficulty urinating.
- Increasing pain.
- Escalating redness, swelling, or discharge from the incision site.
Understanding Post-Hysterectomy Changes
Physical Well-Being
- Menstrual Changes Following a hysterectomy, menstruation ceases. Occasional bloating and symptoms resembling menstrual discomfort may occur.
- Incision Site Expect some discomfort at the incision site for around four weeks. Any redness, bruising, or swelling typically dissipates in four to six weeks. Sensations of burning or itching are common. Numbness around the incision, extending down the leg, is normal and may last approximately two months. Scarring, both internal and external, is to be expected, with laparoscopic surgeries generally resulting in smaller, less visible scars compared to abdominal procedures.
- Hormone Effects if your ovaries remain, there shouldn’t be hormone-related effects. However, if your ovaries were removed, menopausal symptoms like hot flashes may occur. Hormone replacement therapy may be recommended to alleviate these symptoms.
- In cases of a subtotal hysterectomy, some individuals may continue to experience light periods for up to a year post-procedure due to small amounts of endometrial lining remaining in the cervix.
Emotional Well-Being
Emotional responses to a hysterectomy vary based on preparation, the reason for surgery, and whether the problem has been effectively addressed. Feelings of loss are common but typically temporary. Some individuals find that a hysterectomy improves their overall health and well-being.
Menopause After Hysterectomy
Whether menopause ensues after a hysterectomy depends on the retention of your ovaries. If your ovaries remain intact, menopause will not occur immediately. However, if both ovaries are removed, menopause may commence immediately.
Pap Tests After Hysterectomy
In general, routine Pap tests are not necessary after a hysterectomy, particularly for individuals at low risk of cervical cancer. However, individuals who underwent a hysterectomy due to cancer should continue to have vault smears as recommended.
Impact on Sexual Function
A hysterectomy typically does not affect sexual function. However, if ovaries were removed, menopausal symptoms such as decreased libido and vaginal dryness may occur. The use of a water-based lubricant can help manage dryness.
Orgasm After Hysterectomy
Orgasms and ejaculation are still possible after a hysterectomy since the external vaginal organs and pelvic nerves remain intact following a simple hysterectomy.
Changes for Partners
Studies indicate that sexual pleasure remains unchanged for partners after a hysterectomy. In rare cases, such as when a hysterectomy is performed for cancer or prolapse, alterations in vaginal canal shape may result in discomfort, especially during penetration.
Alternatives to Hysterectomy
When a hysterectomy is not medically necessary, alternatives may be considered, based on your specific symptoms or condition. These alternatives may include observation, medication, hormonal preparations or operative procedures to address specific issues (e.g, fibroid removal or myomectomy). For vaginal weakness or uterine prolapse ,pelvic exercises, or the use of a pessary to support the uterus may be advised. Minimally invasive vaginal repair procedures may be employed for vaginal laxity. In cases of heavy bleeding hysteroscopic procedures may be employed to treat local pathologies.
Remember to maintain open and honest communication with your healthcare provider regarding your symptoms and concerns to ensure the best treatment plan. If a hysterectomy is recommended, it is essential to understand the procedure and recovery process thoroughly.