Do I need Hysterectomy? What are the Alternatives
A hysterectomy is a surgical procedure that involves the removal of the uterus, and sometimes the cervix as well. Depending on the medical indication, this surgery may also involve the removal of adjacent organs and tissues, such as the fallopian tubes and ovaries. After a hysterectomy, a woman cannot become pregnant, and she will no longer experience menstrual periods. This procedure is commonly performed to address various conditions affecting a woman’s reproductive system.
Hysterectomy is one treatment option for various diseases and conditions. It may be a life-saving procedure if you have cancer of the uterus or ovaries, or if your uterus is bleeding uncontrollably. In most other cases, a hysterectomy is performed to improve a woman’s quality of life. This is known as an elective hysterectomy. It can relieve pain, discomfort, or heavy bleeding. It’s worth noting that approximately 10% of hysterectomies are done for a cancer diagnosis, while the majority of the remaining 90% are elective hysterectomies. Despite the relatively low lifetime risk of all gynecologic cancers (with uterine/endometrial cancer being the highest at 2.9%), a woman’s lifetime risk of having a hysterectomy is 45%.
For many gynecological issues, there may be alternative treatments available. It’s essential to discuss all your options and their potential side effects with your doctor to make an informed decision about what is right for you.
Different Types of Hysterectomy
- Subtotal Hysterectomy: This procedure removes the uterus but leaves the cervix in place.
- Radical Hysterectomy: Typically done to treat cervical or uterine cancer, this procedure involves the removal of the uterus, cervix, upper vagina, fallopian tubes, and ovaries (parametrium) in their entirety.
- Total or Complete Hysterectomy: This involves removing both the cervix and the uterus (womb).
Different Routes of Hysterectomy
- Abdominal Hysterectomy: It is performed through an incision in the abdominal area.
- Vaginal Hysterectomy: This procedure is carried out through the vaginal route, without any incisions on the belly. It’s often performed to address prolapse of reproductive organs.
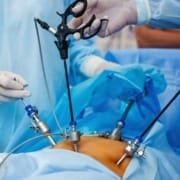
- Total Laparoscopic Hysterectomy: This minimally invasive procedure involves inserting a laparoscope and surgical instruments through several small incisions in the abdomen.
Common Risks of Hysterectomy
- Postoperative Pain
- Urinary Infection, Retention, or Frequency
- Wound Infection, Bruising, and Delayed Wound Healing
Uncommon Risks
- Damage to the Bladder
- Damage to the Bowel
- Pelvic Abscess or Infection
- Venous Thrombosis and Pulmonary Embolism (Blood Clot in Leg/Lung)
- Hernia at the Site of Entry
- Hemorrhage Requiring Blood Transfusion
- Return to the Operating Room Due to Bleeding
- Unexpected Laparotomy (Abdominal Incision)
- Vaginal Vault Dehiscence (Opening) Requiring Re-suturing
When Is Hysterectomy the Only Choice?
While a hysterectomy can effectively alleviate the pain, pressure, and bleeding caused by uterine conditions, it’s crucial to carefully consider the pros and cons of surgery. In some cases, a hysterectomy may become the only viable option, particularly when a woman is diagnosed with cancer of the uterus, ovaries, cervix, or endometrium.
When Is a Hysterectomy Necessary?
Several common reasons may necessitate a hysterectomy:
- Uterine Fibroids: These can lead to pain or heavy periods.
- Excessive Bleeding: Including extremely heavy periods.
- Endometriosis: Which causes pelvic pain.
- Adenomyosis
- Unsuccessfully Treated Pelvic Inflammatory Disease (PID)
- Uterine Prolapse: This involves the uterus sliding from its normal position into the vaginal canal.
- Cancer: Whether it’s in the uterus, cervix, or ovaries.
Making the Decision
The decision to undergo a hysterectomy is complex and depends on various factors:
- Reason for Hysterectomy: Why it’s being considered in the first place.
- Type of Hysterectomy Offered
- Patient’s Preferences: A woman’s wishes for treatment.
- Tolerance for Side Effects or Symptoms
- Alternatives to Hysterectomy
Alternatives to Hysterectomy
There are various alternatives to hysterectomy, depending on the specific condition and patient preferences. Here are some options:
- Lifestyle Changes: Making healthy lifestyle changes can sometimes alleviate symptoms and improve overall well-being.
- Physical Therapy: Physical therapy may be recommended for certain gynecological issues.
- Watchful Waiting: If fibroids are not causing symptoms, a strategy known as “watchful waiting” involves monitoring them with a healthcare provider without opting for surgery unless issues arise.
- Medications and Hormone Replacement: Painful symptoms of uterine fibroids can initially be treated with nonsteroidal anti-inflammatory drugs (NSAIDs). Hormonal drugs that block the production of estrogen and other hormones can be used to halt menstruation and shrink fibroids. However, these medications may have side effects.
- Intrauterine Hormonal Devices: Devices like Mirena can help control heavy bleeding and are a first-line measure for some women.
- Robotic-Assisted Removal of Adhesions: Surgical removal of scar tissue and implants related to endometriosis and adenomyosis can be done using robotic assistance.
- Cystectomy: Removal of ovarian cysts or tumors while preserving healthy ovarian tissues.
- Uterosacral Vault Suspension: A surgical procedure to repair uterine or vaginal prolapse.
- Abdominal Sacrocolpopexy: Repair of vaginal tissue, ligaments, and muscles for vaginal laxity or prolapse.
- Myomectomy: Surgical removal of fibroids only, which can be done through an abdominal operation or laparoscopically.
- Hysteroscopy: A minor surgical procedure involving the insertion of a hysteroscope to treat fibroids within the uterine cavity.
- Uterine Fibroid Embolization (UFE): A minimally invasive procedure that blocks blood flow to fibroids, causing them to shrink or disappear. It is performed by an interventional radiologist and has 90% success rate. It also preserves the uterus.
- Endometrial Ablation: Removal of the uterine lining to reduce bleeding during periods, often resulting in lighter or absent periods.
Who Should Avoid Hysterectomy?
While a hysterectomy is the right treatment for some patients, it’s essential to consider alternatives, especially if you wish to preserve fertility or avoid potential side effects. Here are some reasons why you might avoid a hysterectomy:
- If you want to have children in the future, a hysterectomy is not an option.
- Young women should only consider a hysterectomy as a last resort when other treatments have failed.
- Hysterectomy can have lasting side effects, including vaginal dryness, mood swings, hot flushes, difficulty achieving orgasm, bladder and intestinal changes, emotional issues, and depression.
- If you have cancer of the uterus, ovaries, cervix, or endometrium, a hysterectomy may be necessary.
In many cases, alternatives and less invasive treatments may provide effective relief from symptoms without the need for a hysterectomy.