Ovarian Cysts and Tumors, Symptoms, Causes and Treatment
What are Ovarian Cysts and Tumors?
The ovaries are small organs that play a crucial role in regulating women’s reproductive processes. Typically, women are born with two ovaries, one on each side of the uterus. These small organs come into action during adolescence, producing hormones and regulating the menstrual cycle. While ovarian cysts are a common occurrence and usually harmless, some women may encounter ovarian tumors, which can be more complex. Such tumors warrant a closer examination and potential medical intervention.
Ovarian tumors come in various types, with the possibility of being ovarian cancer. Notably, ovarian cancer often presents minimal symptoms during its early stages. Several factors can contribute to the risk of ovarian cancer, including age, family history, obesity, and the use of fertility drugs.
Ovarian enlargement, characterized by the presence of masses or tumors, can be attributed to various factors, including cysts (such as ovarian and hemorrhagic ovarian cysts), masses known as endometriomas, or tumors (abnormal growths). It’s important to note that the majority of ovarian masses found in girls and young women are non-cancerous. Ovarian cysts are typically linked to hormonal changes and/or the process of ovulation. Meanwhile, ovarian masses like endometriomas are associated with endometriosis, an inflammatory condition where the endometrial glands and stroma are located outside the uterus. The exact causes of both benign and malignant masses remain uncertain. While many of these noncancerous cysts and tumors are asymptomatic, some may lead to pelvic discomfort or pressure.
Natural Resolution and Medical Intervention
In several cases, noncancerous cysts resolve spontaneously. However, when necessary, cysts or tumors can be surgically removed. The procedure may involve one or more small incisions or a single large abdominal incision. On occasion, the affected ovary may also require removal.
Ovarian Cyst Overview
Ovarian cysts, characterized by fluid-filled sacs forming within or on an ovary, are relatively commonplace. The majority of these cysts are benign and tend to regress autonomously. Ovarian cancer typically presents a higher risk in women aged 50 and above. 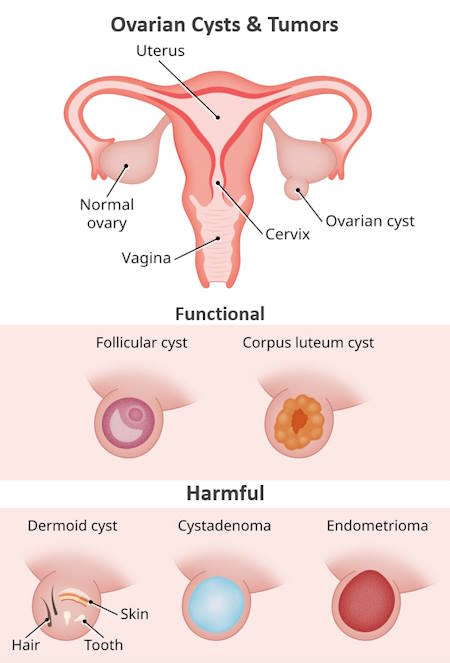
Functional Ovarian Cysts
Functional ovarian cysts originate from the fluid-filled cavities known as follicles within the ovaries. Typically, during each menstrual cycle, a single egg is released from a follicle, which subsequently diminishes. However, if an egg remains unreleased, the follicle may persist, evolving into a larger cyst. These cysts can be a sign that your ovaries are functioning normally. Functional cysts generally shrink over time, usually within two months, without any specific treatment. The majority of functional cysts tend to self-resolve within days or weeks.
Functional cysts are primarily encountered in premenopausal women and rarely develop post-menopause. There are two distinct types:
- Follicular Cysts: These cysts manifest during the egg’s developmental phase within the follicle.
- Corpus Luteum Cysts: These cysts arise from the structure formed after the follicle’s rupture and egg release, known as the corpus luteum. Corpus luteum cysts can occasionally bleed, leading to ovarian enlargement or even rupture, resulting in the release of fluids into the abdominal cavity, causing significant pain.
Functional cysts typically measure less than 5cm in diameter, although some may reach larger sizes and cause symptoms.
Benign Ovarian Tumors
Noncancerous (benign) ovarian tumors usually grow slowly and rarely turn into cancer. The most common types are:
- Benign Teratomas (Dermoid Cysts): These tumors develop from different layers of cells in the embryo and can contain tissues from various body parts like nerves, glands, and skin.
- Fibromas: Fibromas are solid masses made of connective tissue. They tend to be small, usually less than 3 inches in size, and are often found on just one side.
- Cystadenomas: These are fluid-filled cysts that form on the surface of the ovary and may contain some glandular tissue.
- Endometrioma : Endometriosis happens when the lining of the uterus (womb) grows outside of the uterus. These are typically filled with chocolate colored fluid characteristic of endometriosis.
Symptoms
Most of the time, noncancerous ovarian tumors and functional cysts don’t cause any symptoms. But in some cases, they can lead to:
- Occasional dull or sharp pelvic pain
- Irregular menstrual periods or heavy bleeding
- Spotting between periods
- Abdominal discomfort during sexual activity
- Hormone production by certain cysts, affecting periods and potentially causing vaginal bleeding in postmenopausal women
- Pain or tenderness in the pelvic area if corpus luteum cysts bleed
- Sudden and severe abdominal pain due to twisting of the ovary (adnexal torsion)
- Rarely, the buildup of fluid in the abdomen (ascites) or around the lungs (pleural effusion) in conditions like Meigs syndrome, often seen with fibromas or ovarian cancer. Ascites can cause abdominal pressure or heaviness.
- Feelings of fullness or abdominal bloating
- Early satiety (feeling full quickly after eating)
- Changes in urinary and bowel habits
Diagnosis
Doctors may detect cysts or tumors during a routine pelvic exam or if symptoms are present. Imaging tests, like ultrasonography, can also identify these growths, often when looking for other issues.
To confirm the diagnosis, transvaginal ultrasonography (using an ultrasound device inserted into the vagina) is often performed.
A pregnancy test may be done to rule out pregnancy or an ectopic pregnancy (outside the uterus).
If cancer is suspected or if ascites is found, the growth is removed and examined under a microscope. A laparoscope (a tiny camera) may be used for this, inserted through a small incision below the navel.
Blood tests for tumor markers may be done to assess ovarian cancer, but these tests aren’t always reliable for diagnosis and are more useful for tracking treatment progress. CT scan and MRI may be used if cancer is suspected.
Treatment
The approach to treating ovarian masses or tumors depends on the likely diagnosis and the symptoms experienced by the patient. In many cases, ovarian cysts do not produce significant symptoms, tend to resolve on their own, and thus do not necessitate surgical intervention. However, when endometriomas lead to pain, surgical removal becomes necessary. Ovarian neoplasms, on the other hand, continue to grow and typically require surgical intervention. In cases where preoperative assessments indicate a low probability of malignancy, ovarian-sparing surgery (ovarian cystectomy) is performed. This procedure involves removing only the mass or tumor while preserving the normal ovarian tissue. Conversely, if there are concerns about ovarian malignancy based on pelvic imaging and/or ovarian tumor markers, the entire ovary is removed.
For some cysts, regular monitoring with transvaginal ultrasonography may be all that’s needed. In other cases, surgery might be necessary.
Ovarian Cysts
- If ovarian cysts are small, about 2 inches (5 centimeters) or less in diameter, they often disappear on their own without treatment. Periodic transvaginal ultrasonography is used to check if they are going away.
- However, if a cyst is larger than about 2 inches and doesn’t go away, it might require removal. If cancer is a possibility, the entire ovary may need to be removed. In cases of confirmed cancer, the cysts, affected ovary, and fallopian tube are typically removed. For some large cysts that don’t exhibit cancerous traits, monitoring with transvaginal ultrasonography may suffice.
Ovarian Tumors
- Benign tumors like fibromas and cystadenomas usually need treatment.
- When a tumor appears to be cancerous, surgery is performed to assess and potentially remove it. The choice of procedure depends on the tumor’s size and its impact on nearby organs. Two common approaches are:
- Laparoscopy: This minimally invasive procedure involves small abdominal incisions, usually requiring general anesthesia. A small camera is passed through the minimal incision in the abdomen.This approach has minimal side effects ,less need for pain killers, less infections and a shorter hospital stay.
- Laparotomy: A larger incision is made in the abdomen, and this procedure usually necessitates hospital stay.
- Doctors aim to preserve the ovaries when possible by removing only the cyst (cystectomy). However, the complete removal of the affected ovary (oophorectomy) becomes necessary in certain situations:
- Solid tumors like fibromas if cystectomy isn’t possible.
- Cystadenomas.
- Cystic teratomas larger than 4 inches.
- Cysts that cannot be separated from the ovary surgically.
- Most cysts in postmenopausal women that are larger than approximately 2 inches.
Frequently Asked Questions
What is the most common ovarian tumor?
The most prevalent ovarian tumor in young age is Mature Teratoma. This benign tumor typically affects women between their teenage years and forties. It’s often referred to as a dermoid cyst because it has a lining resembling skin, known as dermis.
What is the difference between ovarian tumor and ovarian cyst?
Ovarian cysts and tumors have differences. Cysts are often benign, but in some cases, they might require draining or removal because they can cause troublesome symptoms. Tumors, on the other hand, are generally more solid collections of tissue. They develop when cells start growing uncontrollably or don’t die as they should.
When to Seek Medical Help for Ovarian Cysts?
If you experience sudden, severe pain along with dizziness, fever, or nausea and vomiting, contact a doctor immediately. These symptoms could indicate a ruptured cyst or ovarian torsion (twisting). Without medical attention, heavy bleeding or infection may occur.
Suspecting Ovarian Tumors: What to Expect from my doctor?
When you suspect ovarian tumors, your gynecologist will likely recommend a pelvic exam. During this examination, they’ll check your abdomen for any abnormal growths. In some cases, additional tests like ultrasound or MRI may be ordered. If a tumor is detected, your doctor may perform a laparotomy / laparoscopy to remove it and conduct a biopsy to check for cancer. If cancer is confirmed, chemotherapy and radiation therapy may be necessary to eliminate cancer cells and prevent further growth.
What can I do to reduce the risk of Ovarian Tumors?
There are steps you can take to lower your risk of ovarian tumors:
- Maintain a Healthy Weight: Staying at a healthy weight can reduce the risk.
- Consider Birth Control: Birth control use has been linked to a lower risk of ovarian cancer. Discuss this with your gynecologist.
- Breastfeed: Breastfeeding can lower the risk, and the longer you breastfeed, the more it can help.
- Pregnancy: Having more full-term pregnancies can also reduce the risk of ovarian and fallopian tube cancer.